Wisdom teeth often cause confusion and concern, especially when pain or infection appears. Many people assume that removal is the only option, but in some situations, a wisdom tooth root canal may be considered. Understanding when this treatment is appropriate, how it works, and what it involves can help patients feel more confident about their dental care choices.
This guide explores the wisdom tooth root canal in clear, practical language, covering symptoms, treatment decisions, and what many patients can expect from the process.
Understanding Wisdom Teeth and Their Role in the Mouth
Wisdom teeth are the last teeth to develop, often emerging in the late teens or early adulthood. These third molars sit at the back of the mouth and are sometimes referred to as the last teeth to erupt.
While some wisdom teeth grow in without issue, others cause dental issues due to limited space, awkward positioning, or difficulty cleaning. Partially erupted wisdom teeth and impacted wisdom teeth are especially prone to problems, including infection, gum disease, and tooth decay.
Since wisdom teeth sit close to other teeth and are enclosed by soft tissue and gum tissue, small issues can worsen rapidly when not addressed early.
Can a Wisdom Tooth Need a Root Canal?
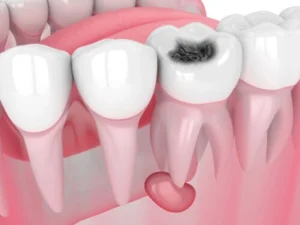 Yes, in certain cases, a wisdom tooth may need a root canal. A root canal treatment focuses on saving a natural tooth by removing infected pulp from inside the tooth. This pulp contains nerves, blood vessels, and connective tissue. When it becomes infected, severe pain, swelling, and sensitivity to hot or cold can occur.
Yes, in certain cases, a wisdom tooth may need a root canal. A root canal treatment focuses on saving a natural tooth by removing infected pulp from inside the tooth. This pulp contains nerves, blood vessels, and connective tissue. When it becomes infected, severe pain, swelling, and sensitivity to hot or cold can occur.
A wisdom tooth root canal is usually considered when the tooth is functional, well-positioned, and contributing to the bite. If the tooth can be properly cleaned and restored, root canal therapy may be the best course rather than immediate tooth removal.
Signs You May Need a Root Canal in a Wisdom Tooth
Recognising symptoms early can prevent complications and support better oral health. Common signs that suggest a wisdom tooth root canal may be required include:
- Persistent tooth pain that does not settle
- Sensitivity to hot or cold temperatures that lingers
- Noticeable swelling in the gums around the wisdom tooth
- Pain when touching the tooth or biting
- Signs of infection, such as swelling, tenderness, or discharge
- Discomfort spreading to adjacent teeth or nearby teeth
In many patients, pain may begin as mild discomfort and gradually worsen. If left untreated, an infected pulp can spread bacteria into the surrounding bone and soft tissue.
Why Wisdom Teeth Are More Complex to Treat
Root canal treatment in wisdom teeth is more complex than in other teeth. These molars often have curved roots, multiple canals, and limited access at the back of the mouth. Advanced techniques and highly skilled dental care are often required to manage these challenges.
Wisdom teeth also sit close to other teeth, which means infection can affect adjacent teeth and gum tissue if not managed properly. This is why careful assessment is essential before deciding on a root canal procedure.
When Tooth Extraction May Be Suggested Instead
Although saving a natural tooth is often preferred, a wisdom tooth root canal is not always the best option. Dentists consider several factors before recommending treatment.
Tooth extraction may be suggested if the wisdom tooth is:
- Severely decayed beyond repair
- Severely damaged or fractured
- Impacted and unable to fully erupt
- Causing repeated infection or gum disease
- Difficult to access for proper cleaning and restoration
In these situations, tooth removal may reduce the risk of ongoing dental issues and support long-term oral health.
Root Canal Versus Tooth Extraction for Wisdom Teeth
 Many patients wonder whether it is better to save or remove a wisdom tooth. Both options have benefits depending on the situation.
Many patients wonder whether it is better to save or remove a wisdom tooth. Both options have benefits depending on the situation.
A root canal can save a natural tooth and maintain chewing function. Tooth extraction removes the source of infection completely but may lead to shifting of other teeth or future restorative needs, such as a dental implant.
The decision depends on several factors, including tooth position, level of decay, and overall oral health.
The Assessment Process Before Treatment
Before any dental procedure, a thorough assessment is carried out. This includes reviewing your medical history, evaluating symptoms, and taking X-rays to examine the root structure and surrounding bone.
X-rays help identify cavities, infected pulp, damaged pulp, and the position of the root in relation to nearby teeth. This step is critical in deciding whether endodontic treatment or tooth extraction is the most suitable option.
What Happens During a Wisdom Tooth Root Canal Procedure
A wisdom tooth root canal follows the same principles as other root canal therapy treatments, with additional care due to the tooth’s position.
Accessing the Tooth Safely
The dentist creates a small opening in the tooth to reach the infected pulp. Local anaesthetic is used, so many patients feel pressure rather than pain during the procedure.
Removing the Infected Pulp
Using specialised instruments, the infected pulp, nerves, and damaged tissue are thoroughly removed from the root canals. This step helps eliminate infection and prevent further spread to nearby teeth or bone.
Cleaning and Shaping the Canals
The canals are cleaned, disinfected, and shaped to prepare them for filling. This process removes bacteria and debris that could lead to future infection.
Sealing with Gutta Percha
Once the canals are thoroughly cleaned, they are filled with gutta-percha to seal the space and reduce the risk of reinfection, before the tooth is temporarily or permanently restored.
Recovery After Root Canal Therapy
After a wisdom tooth root canal, some tenderness or mild discomfort is common for a few days. This usually settles as the surrounding tissue heals.
Patients are often advised to avoid eating on the treated side until the final restoration is complete. Avoid eating very hard or sticky foods during early healing to protect the tooth.
Good dental care at home, including gentle brushing and keeping the area clean, supports recovery and long-term success.
Is a Crown Always Needed After Treatment?
In many cases, wisdom teeth do not need crowns, especially if they are not heavily involved in chewing. However, if the tooth is severely decayed or weakened, additional restoration may be recommended to protect it from fracture.
Your dentist will assess whether restoring the tooth fully is necessary based on function, bite alignment, and overall dental health.
Risks and Possible Complications
Like any medical procedure, a wisdom tooth root canal carries some risks, though complications are not common when performed with care.
Potential issues include:
- Persistent infection if all canals are not fully cleaned
- Temporary swelling or sensitivity
- Difficulty healing due to complex root anatomy
Choosing the most effective course of treatment early reduces the likelihood of complications and improves outcomes.
Long-Term Outlook After Treatment
When successful, a wisdom tooth root canal can last many years. Maintaining oral health through regular dental check-ups, good dental hygiene, and early management of dental issues plays a major role in long-term success.
Patients who address pain, infection, or sensitivity early often avoid more invasive treatments later.
When to Seek Dental Advice Promptly
Do not ignore wisdom tooth pain or signs of infection. Severe pain, swelling, sensitivity to hot or cold, or discomfort spreading through the mouth should be assessed promptly.
Left untreated, infection can spread beyond the tooth, affecting bone, gum tissue, and overall health.
How Wisdom Tooth Anatomy Affects Root Canal Success
Wisdom teeth, also known as third molars, have anatomical features that set them apart from other teeth in the mouth. These differences play a significant role in how predictable a wisdom tooth root canal can be and whether saving the tooth is a realistic option.
One of the main challenges lies in root shape. Wisdom teeth often have curved, fused, or unusually narrow roots. Some have more canals than expected, while others have canals that branch or change direction suddenly. These variations make it harder to fully clean and seal the infected areas, which can influence long-term success.
Positioning also matters. Wisdom teeth sit at the very back of the mouth, which limits visibility and access. Teeth that are tilted, partially erupted, or positioned close to adjacent teeth may be harder to assess and monitor over time. When a wisdom tooth sits too close to nearby teeth or bone, preserving it becomes more complex.
That said, anatomy alone does not rule out treatment. With careful assessment, X-rays, and advanced imaging, a dentist can determine whether the tooth structure supports predictable healing and long-term function.
Age and Healing Considerations for Wisdom Tooth Treatment
Age plays an important role in how the body responds to dental treatment, including decisions around wisdom tooth root canal therapy.
In younger patients, particularly those in their late teens or early twenties, the pulp tissue inside wisdom teeth is often more vital, and the blood supply is stronger. Bone density tends to be lower and healing capacity higher, which may support better outcomes when infection is addressed early.
As patients age, changes occur within the tooth and surrounding structures. The pulp chamber may shrink, canals can become narrower, and bone around the roots may become denser. These factors can make treatment planning more complex and healing slower. Older patients may also have a longer history of dental issues, previous restorations, or gum disease that influences decision-making.
Medical history is another consideration. Conditions that affect healing, immune response, or blood flow can influence whether preserving a wisdom tooth is advisable. Treatment planning must always consider the whole patient, not just the tooth.
The Role of Early Diagnosis in Avoiding Complications
Early diagnosis is one of the most important factors in preventing serious complications related to wisdom teeth. Many problems begin quietly, especially when infection develops deep within the pulp or bone.
Routine dental visits allow dentists to identify cavities, early pulp changes, or subtle signs of infection before severe pain appears. X-rays are especially valuable for detecting problems below the surface, including bone involvement or infection near the root.
Symptom awareness also matters. Sensitivity to hot or cold, swelling, or discomfort that comes and goes can be early warning signs. Ignoring these symptoms often allows infection to progress, increasing the risk of severe pain, swelling, or emergency treatment.
When dental issues are addressed early, treatment options are broader and outcomes are more predictable. Early care often means less disruption, reduced discomfort, and better protection of surrounding teeth and tissues.
How an Infection in a Wisdom Tooth Can Affect Nearby Teeth
Infection within a wisdom tooth does not always stay confined to that tooth. Because third molars sit close to adjacent teeth, bone, and soft tissue, an untreated infection can spread and cause wider dental issues.
 Bacteria from an infected pulp can move into surrounding bone, weakening structural support and increasing the risk of bone loss. Nearby teeth may become sensitive or painful as inflammation spreads through shared tissues. In some cases, infection can affect the roots of adjacent teeth, creating secondary dental problems that require additional treatment.
Bacteria from an infected pulp can move into surrounding bone, weakening structural support and increasing the risk of bone loss. Nearby teeth may become sensitive or painful as inflammation spreads through shared tissues. In some cases, infection can affect the roots of adjacent teeth, creating secondary dental problems that require additional treatment.
Soft tissue is also vulnerable. Swelling, tenderness, and inflammation in the gum tissue can make cleaning difficult, increasing the risk of gum disease and further infection. Over time, this cycle can compromise overall oral health.
Addressing infection promptly helps protect not just the wisdom tooth, but the stability and health of the entire mouth.
Final Thoughts on Wisdom Tooth Root Canal Treatment
A wisdom tooth root canal is not suitable for everyone, but in the right circumstances, it can be a valuable way to save a natural tooth and protect oral health. With careful assessment, advanced techniques, and skilled dental care, many patients achieve relief from pain and infection while preserving function.
Understanding wisdom teeth, recognising symptoms early, and exploring treatment options with a dentist helps ensure the most appropriate and effective outcome. Whether the solution is root canal therapy or tooth extraction, informed decisions support comfort, confidence, and long-term dental well-being.
If you are experiencing wisdom tooth pain, swelling, or signs of infection, the team at Complete Dental can assess your situation and guide you through the most suitable treatment options with clarity and care.
- Coorparoo: 07 3801 6503
- Elanora: 07 5235 8199
Note: Any surgical or invasive procedure carries risks. Before proceeding, you should seek a second opinion from an appropriately qualified health practitioner.
References
- NHS. (2025, February 17). Take care of your teeth and gums. NHS. https://www.nhs.uk/live-well/healthy-teeth-and-gums/take-care-of-your-teeth-and-gums/
- Colgate. (2023, January 9). Gutta percha: What is it and when is it used. Colgate. https://www.colgate.com/en-us/oral-health/root-canals/gutta-percha-what-is-it-and-when-is-it-used
- Krans, B. (2023, February 22). Dental X-rays: Purpose, procedure, and risks. Healthline. https://www.healthline.com/health/dental-x-rays
- Listerine Middle East. (2024). Swollen gums: Causes, treatments & prevention. Listerine-ME. https://www.listerine-me.com/gingivitis/swollen-gums
- Cleveland Clinic. (2025, June 23). Wisdom teeth: Function & location. Cleveland Clinic. https://my.clevelandclinic.org/health/body/23223-wisdom-teeth